Sympathetic nervous system dysfunction symptoms often feel less like doing too much, and more like a body that never fully relaxes. It comes from never fully switching off.
Not always obvious. Not dramatic. Just… constant.
A body that feels alert even in quiet moments. A mind that tries to rest but doesn’t quite land there. And over time, it starts to feel normal. Or at least familiar enough to ignore.
That’s often where sympathetic nervous system dysfunction quietly sits. Not loud. Not labeled. But very present.
What is sympathetic nervous system dysfunction, really?
At its simplest, it means this: the body’s stress response system is overactive and struggling to return to baseline.
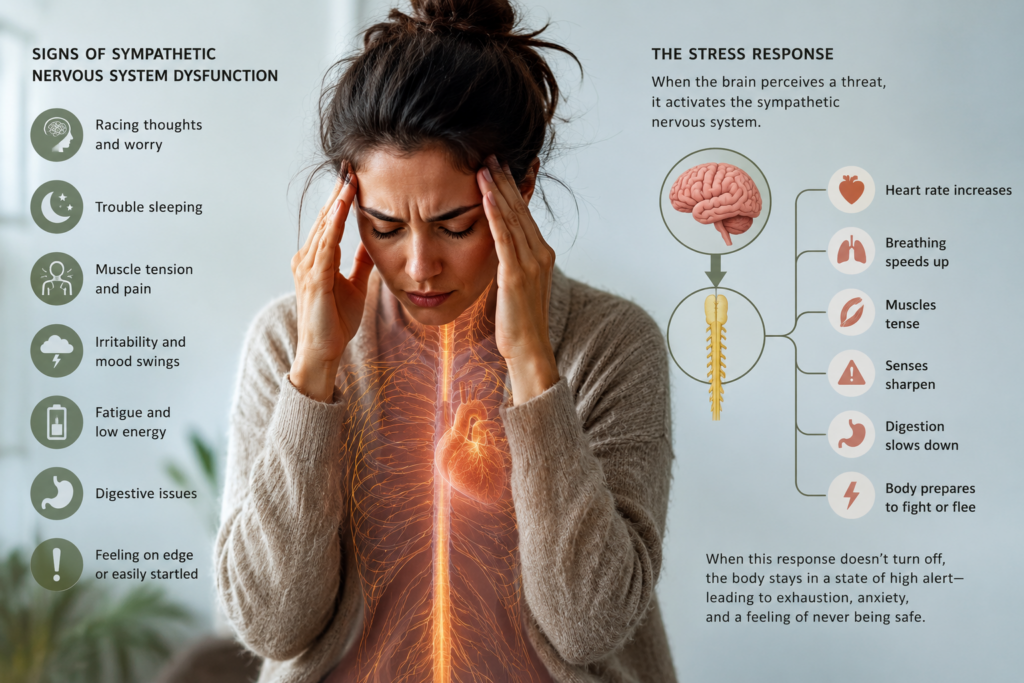
The sympathetic nervous system is responsible for the fight or flight response. It’s designed to protect. When something feels threatening, it prepares the body to react quickly. Heart rate increases. Muscles tighten. Awareness sharpens.
That part works exactly as it should.
The problem begins when that response doesn’t turn off.
Instead of moving from activation back to calm, the system lingers somewhere in between. Not full panic. But not settled either. A kind of low-level activation that becomes the new normal.
According to insights shared on Dual Sympathetic Reset (DSR), this ongoing activation is often tied to how the body processes trauma. Or more accurately, how it sometimes doesn’t.
What Are Sympathetic Nervous System Dysfunction Symptoms People Tend to Miss?
The short answer: they’re easy to dismiss because they don’t always look extreme.
Most people expect something obvious. Something that clearly signals “this is a problem.” But sympathetic nervous system dysfunction tends to show up in quieter, more persistent ways.
There’s a constant sense of tension in the body—one of the more subtle sympathetic nervous system dysfunction symptoms people often overlook. Sleep becomes inconsistent. Falling asleep might take longer. Staying asleep becomes unpredictable.
Some days feel manageable. Others feel oddly overwhelming without a clear reason, another pattern commonly linked to sympathetic nervous system dysfunction symptoms.
There’s also that underlying restlessness. Even in stillness. A quiet but persistent sign that the body hasn’t fully switched off.
It can look like:
- A racing mind that won’t slow down at night
- Sudden spikes of anxiety that don’t seem connected to anything
- Sensitivity to noise, light, or crowded spaces
- Difficulty concentrating or staying present
- Irritability that feels disproportionate
- A subtle but constant sense of unease
None of these, on their own, always feels alarming. Together, though, they start to form a pattern.
And that pattern often gets labeled as stress. Or anxiety. Or burnout.
Sometimes that label helps. Sometimes it doesn’t go far enough.
Why does trauma affect the nervous system like this?
The direct answer: trauma can keep the body’s survival system switched on long after the event has passed, often contributing to ongoing sympathetic nervous system dysfunction symptoms.
When something overwhelming happens, the body reacts instantly. That’s not a flaw. It’s protection.
But if the experience isn’t fully processed, the nervous system can hold onto that activated state. Not consciously. Not as a memory someone actively revisits. More like a background setting that never resets—one of the core patterns behind sympathetic nervous system dysfunction symptoms.
This is where the conversation begins to shift.
There’s growing discussion around reframing PTSD as a physical injury rather than only a psychological condition. The idea of Post-Traumatic Stress Injury (PTSI) reflects that shift. It focuses on what’s happening in the body, not just the mind.
Some of that perspective is explored further in trauma-focused research highlighting how biological responses play a central role in ongoing symptoms.
For a broader clinical understanding, the National Institute of Mental Health’s overview of PTSD explains how trauma affects both brain function and physical response systems.
Still, even those explanations can feel a bit distant until the experience becomes personal.
Because when the body feels unsafe, logic doesn’t always settle it.
Why doesn’t the fight or flight response turn off?
Because the body isn’t always responding to the present moment. It’s responding to what it has learned to expect—one of the underlying drivers of sympathetic nervous system dysfunction symptoms.
That’s the quiet complication.
The nervous system isn’t making a mistake. It’s doing what it was trained to do. It stays alert because, at some point, that alertness felt necessary.
Over time, though, that constant readiness becomes exhausting—often showing up as persistent sympathetic nervous system dysfunction symptoms.
And here’s where things get a bit frustrating for many people.
Understanding the cause doesn’t always change the feeling.
Someone might know they’re safe. They might logically understand that the threat is gone. But the body… doesn’t quite agree.
That disconnect is often where traditional approaches feel incomplete.
Why do some treatments feel like they’re not enough?
Because many approaches focus on thoughts and emotions, but not directly on the body’s stress response system.
Therapy can help process experiences. It can bring clarity. It can reduce the emotional weight of certain memories.
Medication can help manage symptoms. It can create stability.
But if the sympathetic nervous system dysfunction remains unaddressed, that underlying state of activation can continue.
That’s why some people describe a strange split. They understand their trauma. They’ve worked through it mentally. And yet, their body still reacts.
That’s not failure. It’s a clue.
It suggests that healing may need to include the body, not just the mind—an idea increasingly supported by research from the National Institute of Mental Health, which highlights how trauma affects both brain and body.
What does it mean to “reset” the nervous system?
In practical terms, it means helping the body return to a state where it no longer feels constantly threatened.
There isn’t just one path to that.
Some approaches focus on gradual regulation. Breathwork. Somatic therapies. Techniques that build awareness and gently guide the body back toward calm.
Others take a more direct route.
Procedures like the one described in Dr. Eugene Lipov’s work aim to influence the sympathetic nervous system more directly. The idea is to interrupt that persistent stress signal and allow the system to recalibrate.
For those exploring options beyond medication, this becomes part of a larger conversation around non medication treatment for trauma-related symptoms.
Not as a replacement for everything else. But as an additional layer.
Something that addresses the physical side of the experience.
Who is this most relevant for?
Anyone who feels like their body is constantly “on,” even when life doesn’t seem to justify that level of stress.
This can include people who have experienced clear traumatic events. But it also includes those who have lived through prolonged stress, pressure, or instability.
Sometimes the source is obvious.
Sometimes it isn’t.
Either way, the pattern tends to look similar. A system that struggles to settle. A sense of tension that doesn’t fully release.
And a growing awareness that something deeper might be at play.
What should someone consider before seeking treatment?
Clarity matters here.
Not every symptom points to nervous system dysfunction. And not every person will need the same approach.
It helps to start with understanding. Paying attention to patterns. Noticing when the body feels activated and what might be triggering it.
From there, exploring options becomes more grounded.
Some may benefit from therapeutic support. Others might look into physiological approaches. In certain cases, a combination works best.
The key is recognizing that there isn’t a single path.
But there is a direction.
A quieter way to look at it
There’s something almost reassuring about realizing that the body isn’t working against itself.
It’s responding. Protecting. Adapting.
Even if the response no longer fits the current situation.
That shift in perspective doesn’t fix everything overnight. But it softens the frustration a bit. Makes space for a different kind of curiosity.
Not “what’s wrong,” but “what is the body trying to do?”
And from there, things begin to change. Slowly, sometimes. Unevenly. But change nonetheless.
IMAGE
Sympathetic nervous system dysfunction doesn’t usually arrive with a clear label. It builds quietly. Settles in. Becomes part of daily life before anyone questions it.
But once it’s recognized, it’s hard to ignore.
Because suddenly, the patterns make sense.
The constant alertness. The fatigue. The feeling of being unable to fully relax.
Not random. Not imagined.
Just a system that hasn’t had the chance to reset yet.
If this feels familiar, it might be worth exploring what your body is holding onto—and what it might need to finally reset. 👉 Start the conversation here!

